Objective: To establish the relationship between sleep duration, nutritional status and caffeinated beverage consumption patterns in school-age Chilean children. Method: The study was conducted in 805 schoolage children, between 6- and 10-years old from 6 neighborhoods in Santiago, Chile. Parents completed a questionnaire, which assessed sleep duration, physical activity and food intake. Anthropometric measurements were completed for children. Results: 52.6% of school-age children were obese and 46.4% slept the recommended amount (≥10 hours). Normal weight subjects slept significantly more hours than obese participants, 9.8 ± 0.9 vs. 9.6 ± 0.9, respectively. Sleep duration during the week was inversely associated to obesity (OR: 3.5, 95% CI 1.3-9.2). Children drank the following beverages at night: caffeinated soft drinks (52.2 %), coffee and/or tea (32.6%) and 21.2 % both soft drinks and coffee tea caffeine beverages Conclusion: Over half of this sample of school-age Chilean children slept less than the recommended (≥10 hours) amount, with obese participants sleeping less than normal weight subjects. The intake of caffeine products in particular, caffeinated soft drinks,was higher during the night in both groups.
Key words: Sleep, obesity, nutritional status, caffeine.
Objetivo: establecer la relación entre cantidad de sueño, estado nutricional y consumo de cafeína en escolares Métodos: El estudio fue realizado en 805 escolares, entre 6 a 10 años de 6 comunas de Santiago de Chile. Los padres completaron las encuestas de sueño, actividad física y consumo de alimentos. A los escolares se les realizó una evaluación antropométrica. Resultados: El 56,2% de los escolares era obeso, el 46,4% dormía menos de lo recomendado (≥10 horas). La cantidad de sueño fue significativamente mayor en los escolares normopeso que en los obesos 9,8 ± 0,9 vs 9,6 ± 0,9, respectivamente. La cantidad de sueño durante la semana fue inversamente asociada a obesidad (OR: 3,5; 95% CI 1,3-9,2). Los escolares bebían en la noche antes de dormir: bebidas carbonadatas con cafeína (52,2%), café y/o té (32,6%) y un 21,2% ambos tipos de bebidas. Conclusión: Más de la mitad de esta muestra de niños en edad escolar, dormia menos de la cantidad recomendada (≥ 10 horas), los escolares obesos dormían menos de sujetos de peso normal. Además se observa una ingesta en la noche de bebidas carbonatadas con cafeína elevada en ambos grupos.
Palabras clave: Sueño, obesidad, estado nutricional, cafeina.
Facultad de Ciencias de la Salud. Universidad San Sebastián. Chile.
Colegio de Nutricionistas Universitarios de Chile.
Childhood obesity is considered a worldwide health problem (1). It increases the risk of the other diseases such as diabetes, dyslipidemia, arterial hypertension and has cardiovascular consequences in adulthood (2). In the last 2 decades, Chile has undergone an epidemiological transition, where pediatric under-nutrition was replaced by overweight and obesity (3). The main strategy for the prevention and treatment against this epidemic has been a healthy diet and physical activity (4). Results of interventions, however, have not been completely effective or positive (1,4,5). Interventions that address other risks factors are needed to reduce obesity and improve intervention results. Some studies have shown an association between reduced sleep duration and childhood overweight, especially in young children (6-8).
Sleep behavior, a healthy diet and physical activity have an important role in the physiological processes of growth, development and health (9). Short sleep duration is related to changes in levels of leptin, ghrelin and cortisol, in addition to glucose tolerance and insulin sensitivity (10). Additional studies have confirmed also that slept deprivation has an impact on increased hunger sensation and daytime appetite (11,12).Thus, short sleep duration is related to the risk of obesity (7). Encouraging adequate sleep as part of an intervention may be novel, effective and complementary to encouraging healthy eating habits and physical activity for the prevention and treatment of obesity (13). In recent years, an increasing number of population studies on the association between sleep and obesity among children have become available. However, similar information is not available for a pediatric large Chilean population or studies that evaluate the association between caffeine beverages and the sleep duration. Therefore, the aim of this study was to establish the relationship between sleep duration, nutritional status and caffeinated beverage consumption patterns in school-age Chilean children.
Study Population: Twelve primary schools with similar socio- economic characteristics from Santiago, Concepción and Valparaíso, Chile.Participated in the study between August 2014 and October 2015. The sample size was calculated based on a previous study (6) and was powered to detect a difference in sleep duration between normal and obese participants of 0.5 hour with a standard error of α=0.05 and 0.9 power.
Inclusion criteria included being between 6- and 10-years old; enrolled in the test school the day of the evaluation, and not being currently treated for sleep disturbance or depression. A total of 887 school-age children between 6- and 10-years old were approached to participate in the study and 805 completed the questionnaires (90.7%). All parents or caregivers provided signed informed consent and children provided informed assent before participation. The institutional review board at the Universidad San Sebastián, Chile approved this study.
Anthropometric Measurements: Trained personal measured body weight and heigh. Weight was measured without shoes or belts in light clothing, and recorded to the nearest 0.1 kg with a digital scale (Seca 813 digital electronic floor scale). Height was measured with a stadiometer to the nearest 1 mm without shoes. WC was measured standing with a non-elastic tape, which was applied horizontally midway between the lowest rib margin and the iliac crest. Body Mass Index (BMI) was calculated as weight (kg)/height (m2). The used BMI reference was the National Center for Health Statistics/Centers for Disease Control and Prevention 2000 Growth Charts (14), which has been endorsed by the Chilean Ministry of Health for its use. Children were classified as obese if their BMI was >95th percentile, non-obese if the BMI was >10th <85th percentile and overweight if the BMI was ≥85 th ≤ 95 th but this group was not considered in our study.
Sleep Duration: Parents were asked to complete the 22-item Pediatric Sleep Questionnaire (PSQ) about their children. The PSQ provides high validity and sensitivity greater than 0.8.
Eating and Physical Activity Habits: Parents were asked about the contents of the last meal of the day, specifically caffeine intake. They were also asked to report the daily physical activity habits of their children. Adequate sleep duration was definedas sleep ≥10 hours per night (8).
Statistics: Data was entered using Excel. Normality of continuous variables was tested using the Shapiro-Wilk goodness of fit test. For normally distributed variables we used the Student t-test and the Mann-Whitney U test was used for non-normally distributed variables. Logistic regression was used to test the relationship between sleep duration, caffeine intake, physical activity and the dependent variable-nutritional status. The α was set as <0.05 for statistical significance. We analyzed data using SPSS version 19.0, Chicago, IL.
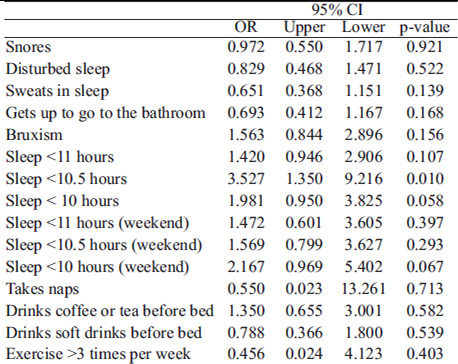
We studied 805 school-age children of which 57% were boys; 47.4% were normal weight (n=382) and 52.6% were obese (n=423). Table 1 shows differences in weight, height and BMI by nutritional status. Fortysix percent of students slept the recommended amount per night (≥10 hours). On weekdays normal weight children slept significantly more than obese students: 9.8 ± 0.9 hours vs 9.6 ± 0.9. Differences did not persist for the weekend. Normal weight girls sleep more hours on weekdays and on weekends (p<0.05). This differs from boys who only had significant differences for the weekend (p<0.05). We found no sex differences in sleep duration during the week and on the weekend.
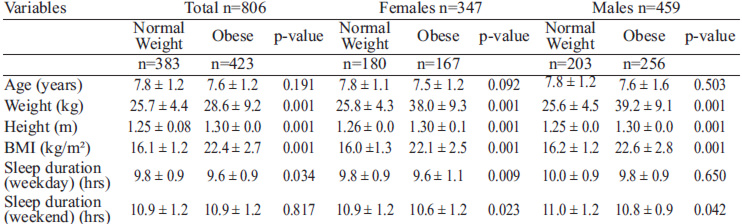
Comparing sleep duration on weekdays by nutritional status and age among girls (Figure 1) we found that as age increased, sleep duration decreased. Six and 7-year old girls sleep significantly more compared to 10-year old girls. Normal weight girls ages 8 and 9 slept significantly more than obese girls of the same ages. We saw similar trends at other ages, but these did not reach statistical significance. We found no differences in sleep duration on the weekend.
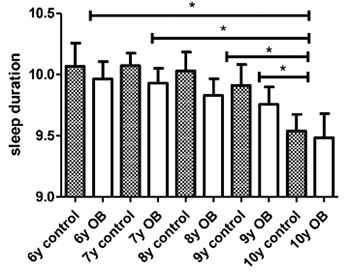
Figure 2 shows that for boys between 6 and 10 years, as age increases, sleep duration decreases (p<0.05). These differences were not observed for the weekend. We found no differences between normal weight and obese boys of the same age with respect to sleep duration.
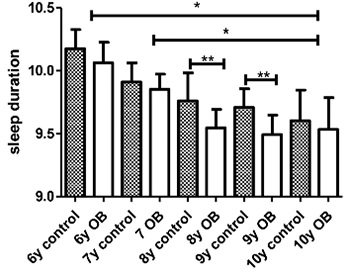
Table 2 shows that sleeping <10.5 hours per night on a weekday was associated with greater odds of obesity (OR: 3.5, 95%CI 1.3-9.2). We found no other significant associations with obesity risk: sleep duration <10 or 11 hours, consumption of caffeine before bed, exercise and others (all p>0.05).
According to parent report, 32.6% of children drank coffee and tea after 8PM, 52.2% drank soft drinks and 21.2% regularly drink coffee, tea or soft drinks before bed. With respect to physical activity, only 20.4% of students reach the recommended amounts of ≥ 3 times per week for ≥ 30 minutes, with no significant differences by nutritional status. Two percent reported never exercising.
Among other behavioral changes in industrialized countries, a decrease in total sleep duration has been noted (13). Adolescents all over the world use computers and watch television for prolonged periods, postponing sleep onset and thus decreasing total sleep duration16. In the current study we observed that obese students slept significantly less during the week than normal weight participants, but no differences were found on the weekend. Both groups responded to the sleep restriction during the week by compensating on the weekend. Observational studies conducted among children have shown sleep duration is negatively associated with BMI and obesity risk (6,8). Chen (5) observed that children who slept <10 hours had a 58% higher risk of overweight or obesity (combined OR=1.58; 95% CI 1.26-1.98). For every additional hour of sleep, the risk of overweight/obesity was reduced by 9% (OR=0.91; 95% CI 0.84-1). This result is similar to that in our study in which sleeping <10.5 hours during the week was associated with obesity (OR: 3.5, 95% CI 1.3-9.2). In a study conducted among Chinese adolescents, researchers showed that short sleep duration was significantly associated with greater adiposity and less lean mass in females (15). Another study demonstrated that sleeping more in the schoolage period is a protective factor for obesity (OR=0.2, 95% CI 0.08-0.85) (9). The association between sleep duration and obesity and sex differences is supported by several studies (13), however we did not find these differences in our analysis. One possible explanation could be that girls are less affected by sleep duration than boys. From an evolutionary perspective, boys may be more vulnerable to environmental stress in childhood, compared to girls (16).
A national survey conducted in the U.S. (2005) showed that 45% of adolescents sleep less than the recommended amount (8 hours or more per night) and 31% are on the border. We found similar values in our study (46%). In our sample of school-age children, we also found that as age increased, sleep duration decreased. Our findings are in line with those of a representative sample of U.S. adolescents conducted by the National Sleep Foundation in 2006 that found that sleep duration was primarily decreased because subjects were going to bed later (17).
A recent study has reported a positive association between physical activity and increased sleep duration in children (18). However we did not find any association between physical activity and sleep duration, albeit the higher sedentary behavior in our sample (79.6%) compared to other studies conducted in school-age children (11,19).
Caffeinated and soft drinks were consumed regularly in both groups before bed, but is not possible to determine is this consumption has a possible disruptive role in sleep duration in obese children.
Strengths of this study include having a representative sample of public school children in Santiago and highly trained personnel carry out the anthropometric measurements. Several limitations must also be mentioned. Our study is cross-sectional, thus causality cannot be determined. We used self-reported measures to determine sleep duration, physical activity, and eating habits. This methodology may have introduced some bias. A final limitation is that screen time (television and/or computer) was not assessed. We consider this narrow age because Tanner staging assessment was not allowed to assess by school rules, hence a puberty assessment in this group could not be done. This is a limitation of our study.
Our results show that short sleep duration during the week (<10.5 hours) is associated with obesity in 6- to 10-year old school children and that obese children sleep less during the week compared to their normal weight peers. Further research is needed to understand the impact of lack of sleep on children obesity, but also public health obesity interventions should include messages associated with adequate sleep duration in children.
For their time and helpful suggestions, we thank all of the teachers that collaborated on this project.
Recibido: 10-09-2016
Aceptado: 21-11-2016