Iodine is an essential constituent of thyroid hormones (TH). TH actively take part in critical periods of brain development during embryonic, fetal and postnatal stages. Therefore the absence of TH or iodine in these critical periods produces an irreversible brain damage. In fact, it is known that iodine deficiency is the leading cause of preventable brain damage worldwide. Because of the physiological adjustments during pregnancy iodine requirements increase significantly from 150 μg per day in non-pregnant adult women to 250 μg per day. Moreover, recent epidemiological studies around the world show that iodine intake during pregnancy is insufficient in many countries, even in developed countries like Australia, Spain and Italy. In the present work an overview of the importance of iodine nutrition during pregnancy is given.
Key words: Pregnancy, thyroid hormones, nutrition, iodine.
El yodo es un nutrimento constituyente indispensable de las hormonas tiroideas (HT). Las HT participan activamente en periodos críticos del desarrollo cerebral durante las etapas embrionaria, fetal y posnatal. Por lo tanto la ausencia o deficiencia de las HT o de yodo en estas etapas del desarrollo produce un daño cerebral irreversible. De hecho, se sabe que la deficiencia de yodo es la principal causa de daño cerebral prevenible en el mundo. Debido a los ajustes fisiológicos propios de la gestación los requerimientos de yodo se incrementan notablemente, pasando de 150 μg al día en la mujer adulta no gestante a 250 μg al día durante el embarazo. Por otra parte, estudios epidemiológicos recientes hechos en todo el mundo muestran que el consumo de yodo durante la gestación es insuficiente en varios países; incluso en países desarrollados como Australia y España e Italia. En la presente revisión se da un panorama general de la importancia del consumo adecuado de yodo durante la gestación.
Palabras clave: Gestación, hormonas tiroideas, nutrición, yodo.
https://doi.org/10.37527/2012.62.3.002
Departamento de Investigación Biomédica, Facultad de Medicina de la Universidad Autónoma de Querétaro. Querétaro. México.
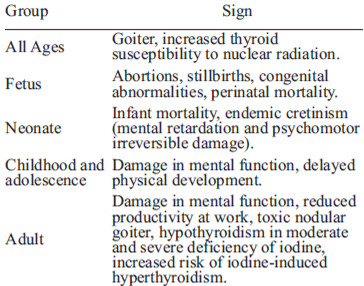
The role of iodine during pregnancy is of great interest because this halogen participates in the development of the central nervous system during embryonic, fetal and postnatal stages (1-3). Iodine is an essential constituent of thyroid hormones (TH), thyroxine and triiodothyronine, thus its deficiency gives rise to a group of diseases generically called iodine deficiency disorders or IDD (4). Table 1 shows a list of IDD, which notably include conditions involving neurodevelopment, brain function and reproduction. Currently, it is considered that iodine deficiency is the leading cause of preventable brain damage in the world (4, 5). In this regard, it is estimated that more than 2 billion people have inadequate iodine consumption (5). For the eradication of iodine deficiency two fundamental strategies have been established, universal salt iodization and continuous epidemiological surveillance (6). Universal salt iodization implies that all salt used for human consumption (table salt and food industry) and livestock must be iodized (6). Epidemiological surveillance mainly consists of periodically assessing the concentration of iodine in table salt, in addition to the determination of the consumption of iodine, which is measured by the urinary iodine concentration (UIC). UIC surveillance must be performed in children between 6 and 12 years of age, and this monitoring is recommended every five years (6).
Pregnant women are vulnerable to iodine deficiency because this physiological condition significantly changes thyroid economy in relation to non-pregnant women (7). Among the most significant changes in thyroidal physiology during pregnancy are the following (7, 8): 1) an increased renal clearance of circulating iodine due to an increase in glomerular filtration rate; 2) an increase in serum thyroxine-binding globulin (TGB) generated by the increase in circulating estrogens, which in turn decreases free thyroxine and consequently increases the levels of thyroid stimulating hormone (TSH), directly stimulating TH synthesis by the thyroid gland; 3) an increase in TH synthesis by chorionic gonadotropin (hCG), due to its binding and activation of the TSH receptor by its similarity to this hormone. These three phenomena result in an increase of up to 50% of circulating TH in pregnancy compared to nonpregnant women. All these changes in thyroid physiology during pregnancy have resulted in an increase in iodine requirements. Table 2 shows the recommended daily iodine intake by age group. During the first trimester of pregnancy the fetus depends on maternal thyroxine provided transplacentally; and at the last stage of pregnancy the fetus can synthesize its own TH, however still depends on the iodine transferred by the mother. Studies in laboratory animals clearly show that severe iodine deficiency during pregnancy causes maternal hypothyroxinemia that directly affects brain development in the offspring (2). In humans it is established that the first trimester of pregnancy is the point of greatest vulnerability to iodine deficiency (8).
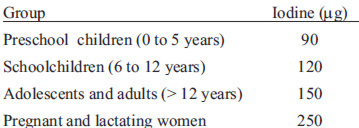
TH have an important role in neurodevelopment (2, 3). They take part in neurogenesis, neuronal migration, myelination and cortical maturation. Such effects of TH in the brain occur at critical periods of development, therefore its deficiency during embryonic, fetal and postnatally at the first few months of life cause irreversible alterations on psychomotor development whose ultimate expression is endemic cretinism (mental retardation and psychomotor irreversible damage) (2-4).
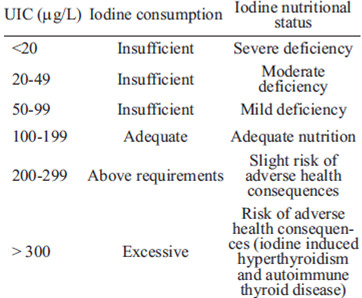
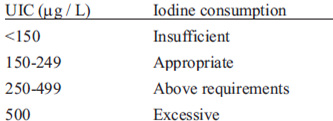
Currently it is agreed that the best indicator for assessing iodine nutritional status is through the median UIC obtained from casual urine samples of a representative sample population (6). Tables 3 and 4 show the epidemiological criteria for categorizing iodine nutritional status by using the median UIC in schoolchildren and pregnant women, respectively. Median UIC in schoolchildren between 6 and 12 years of age is the mainly indicator of iodine nutrition in a general population because it usually reflects the iodine intake adequately (5, 6).
Several countries in recent years have analyzed the iodine nutritional status during pregnancy (see Table 5) (9-25). On one hand, it has been shown that countries without a program of universal salt iodization have less than optimal iodine nutrition during pregnancy (for example Bosnia and Herzegovina, India and Thailand) (9-11). On the other hand, countries like Australia and Iran, with programs of universal salt iodization, show that this type of program may not be sufficient to reach the optimal iodine intake (12-14).
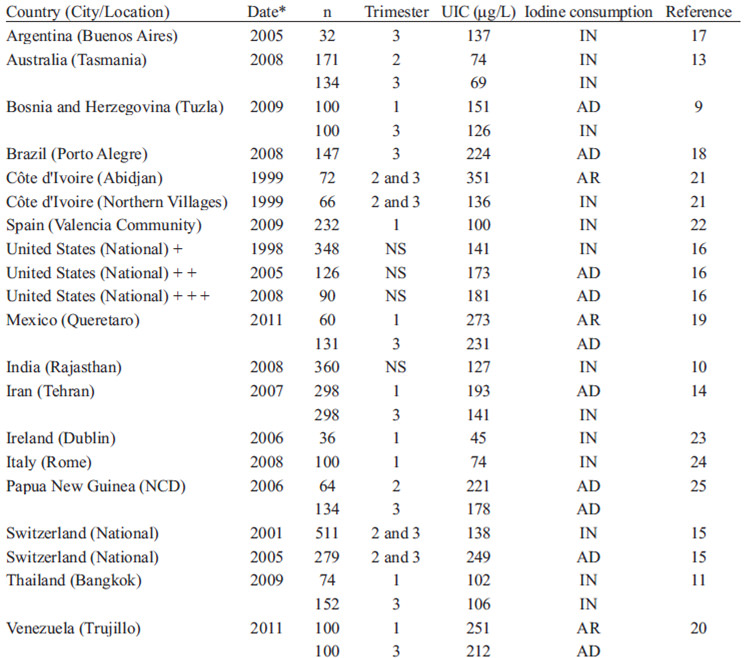
A study in Tasmania showed that the addition of iodine to salt and bread effectively corrected the deficiency of this halogen in the general population; however this strategy was not effective in correcting the insufficient iodine intake during pregnancy (12). In contrast, countries like Switzerland and the United States of America without programs of universal salt iodization reach an adequate iodine consumption (15, 16). These developed countries, however, have permanent monitoring systems that allow the implementation of corrective actions on its population in case of deficiency. In the United States of America there has been detected a significant reduction in UIC in the last 40 years (Table 5) (16). It is noteworthy that the current UIC values are close to the minimum value of iodine sufficiency (see Tables 4 and 5). In fact, the American Thyroid Association recommends to people of the United States of America and Canada that pregnant women should receive 150 μg of iodine in vitamin supplements (1). In Latin America, countries like Argentina, Brazil, Mexico and Venezuela have recent data about iodine nutrition during pregnancy in some regions (17-20). In Argentina (Buenos Aires) the median of UIC was < 150 μg/L whereas in Brazil (Porto Alegre), Mexico (Queretaro) and Venezuela (Trujillo) there was a median UIC >150 μg/L. In all these Latin American countries the universal salt iodization is mandatory (26).
In addition, there is a considerable decline in UIC at the end of pregnancy; several countries like Bosnia and Herzegovina, Iran and Thailand have exhibited this type of behavior (9, 11, 14). The reduction in median UIC at the end of pregnancy is most evident in places where there is a clear iodine deficiency (13). A study in Tasmania showed that at the beginning of pregnancy a 22% of samples had UIC levels < 50 μg/L and 40% at the end (13). This decline could suggest a depletion of iodine storage due to its consumption by the maternal-fetal binomial, its renal elimination and/or by inadequate dietary compensation.
Several studies have showed that the use of the median urinary iodine between 100-199 μg/L in schoolchildren as an indicator of iodine nutrition is not useful as an indicator of adequate intake of iodine during pregnancy in the same regions (5, 6, 10-12, 15-17, 20, 21). In Table 6, as an example, is shown a comparison between median of UIC of schoolchildren and pregnant women in three studies performed in Latin American countries, Argentina (Buenos Aires), Mexico (Hidalgo) and Venezuela (Trujillo) (17, 20, 27, 28). It was found that in Buenos Aires the iodine intake is adequate in schoolchildren but insufficient in pregnant women; whereas in Trujillo a Venezuelan Andean region the iodine intake is adequate in both groups. The WHO, UNICEF and ICCIDD have appealed to the importance of regular monitoring of iodine nutrition during pregnancy and not just in schoolchildren (6).

International agencies recommend that each country should have its own studies on iodine nutritional status in vulnerable populations with the aim to make decisions and public policies based on well founded information (6). In Mexico, very little is known about the consumption of iodine in both schoolchildren and pregnant women. In this regard, the latest national nutrition survey which collected data on iodine nutrition was performed in 1999 and showed a median UIC, in schoolchildren and non-pregnant women, of 231 and 281 μg/L, respectively (29). Both data indicate a consumption of iodine above requirements. However, a study of Castañeda et al. (27) published in 2002 revealed that pregnant women in three localities of the Mexican state of Hidalgo: Pachuca (capital city), Ixmiquilpan (rural area without endemic goiter) and Huejutla (rural area with endemic goiter), showed a median UIC of < 150 μg/L, indicating insufficient iodine intake (Table 6). While in schoolchildren the median UIC was >100 μg/L in Pachuca and Ixmiquilpan, and <100 μg/L in Huejutla (Table 6) (28). In contrast, nine years later, our research group conducted a study on iodine nutritional status in 294 pregnant women in the state of Queretaro, Mexico, and found an overall median UIC of 260 μg/L (19). Our recent data in contrast to those of Hidalgo indicate an iodine intake above requirements in pregnant women. This discrepancy could be explained because of the development of an extensive program of universal salt iodization in Mexico. Currently it is estimated that 80% of the table salt consumed in Mexico contains between 20 and 40 ppm of iodine, and only around of 10% of this salt contains less than 15 ppm of iodine (30).
The universal salt iodization is the most cost-effective strategy to guarantee iodine consumption in general population (6). At present the minimal iodine concentration recommended for table salt is 15 ppm. In this regard for a non-pregnant woman which only iodine source is table salt, 10 g of table salt are needed daily to reach the recommended consumption (150 μg) (6). This implies the consumption of approximately 17 g of table salt for a pregnant woman in order to reach its recommended daily intake (250 μg). Considering the current global trend of reducing salt intake of 10 g/day per capita to less than 5 g/day in order to prevent cardiovascular diseases (31), it is very important to adequately monitoring iodine intake in pregnant women. It is essential not to jeopardize the sufficiency of iodine intake by the reduction of salt intake. As alternatives it should be considered to increase the minimal concentration of iodine in table salt or to establish additional iodine supplementation (multivitamin) in pregnant women. In this regard, it has been documented that salt restriction may compromise iodine intake in pregnant women (9). Larger studies are needed in all the countries to identify patterns of iodized salt intake, and to evaluate other iodine food sources to ensure an adequate iodine intake.
In relation with iodine metabolism in pregnant women with preeclampsia (PE), to our knowledge there is only one study that analyzed UIC (32). This study showed that UIC of women with severe PE is lower than in normal pregnant women, 42.5 ± 27 μg/L versus 208 ± 64 μg/L. This same group found that the concentration of triiodothyronine and iodine in serum, and the concentration of iodine in placenta of women with severe PE were lower than in normal pregnant women (32-34). Indeed, several studies suggest that the placenta may act as a storage place for the supply of iodine to the fetus (35). The previous data suggest that pregnant women with PE have a significant degree of iodine deficiency. In contrast, it has been reported that iodine concentration in blood from the umbilical cord of women with PE is higher than in healthy pregnant women (33). This suggests an adjustment in the physiological mechanisms that favor the passage of iodine to the fetus. In this regard, the supply of iodine to the fetus depends not only on the iodine intake in the mother, but also on the ability of iodine to cross the placenta and on its incorporation into TH by the fetus (35).
Adequate iodine intake during pregnancy is essential to ensure proper brain development and its deficiency in critical periods generates irreversible damage. Iodine metabolism during pregnancy is different from the non-pregnant woman, and this physiological scenario should be taken in account for an adequate nutritional assessment. The UIC determination in the general population for the monitoring of iodine consumption is essential for the design and application of policies directed to ensure an adequate iodine intake. The use of iodine supplementation (multivitamins) in pregnancy should be considered specially when the consumption of table salt is reduced.
This work was partially supported by grants: FOMIX-QRO-2009-C01-117897 and PROMEPPTC-094.
Recibido: 29-05-2012
Aceptado: 04-09-2012