Publicado: 21/06/2024
Introduction: Child health is conditioned by the circumstances of pregnancy, childbirth, and early life. Objective: To describe the maternal and neonatal characteristics of live births (LBs) in the Information System on Live Births of Santa Catarina (SC), Brazil. Materials and methods: A cross-sectional study describedthe maternal and neonatal characteristics of 940,059 LBs, from 2010 to 2019. Pearson’s chi-square test and Fisher’s exact test were conducted, with a statistical significance level of p < 0.05. Results: The mean values of maternal age, number of live children, and number of fetal deaths as well as abortions were 27.1 years, 0.9, and 0.2, respectively. The averages of the number of gestation weeks, number of prenatal consultations, the start date of the prenatal care, and birth weight were 38.5 weeks, 8.1 months, 2.5 monthsand 3,217.1 grams, respectively. Low birth weight (LBW) was prevalent among mothers without education (p < 0.001), including those without prenatal visits (p < 0.001). A higher prevalence of being underweight was observed among female neonates (p < 0.001) and with a maternal age of ≥ 40 years (10.8%; p < 0.001) compared to newborns with good vitality. Newborns with good vitality had a low prevalence of underweight (p < 0.001). The frequency of the variables studied increased, comparing the beginning and end of the period and whether the differences are statistically significant. Conclusions: The study draws attention to the need for interventions to improve the indicators that determine LBW. Arch Latinoam Nutr 2024; 74(2): 74-82.
Keywords: Live birth, health information systems, vital statistics, low birth weight.
Introducción: La salud infantil está condicionada por las circunstancias del embarazo, parto y primeras etapas de la vida. Objetivo: Describir las características maternas y neonatales de los nacidos vivos en el Sistema de Información de Nacidos Vivos de Santa Catarina, Brasil. Materiales y métodos: Estudio transversal describiendo las características maternas y neonatales de 940.059 nacidos vivos entre 2010 y 2019. Se realizó la prueba de chi cuadrado de Pearson y exacta de Fisher y se estableció p < 0,05. Resultados: Los valores medios para la edad materna, el número de nacidos vivos y el número de mortinatos y abortos espontáneos fueron 27,1, 0,9 y 0,2, respectivamente. Las medias del número de semanas de gestación, el número de visitas prenatales, la fecha de inicio de la atención prenatal y el peso al nacer fueron 38,5 semanas (DE 2,2), 8,1 meses, 2,5 meses y 3 217,1 gramos, respectivamente. El bajo peso al nacer (BPN) fue prevalente entre las madres sin estudios (p < 0,001), incluidas las que no acudieron a una cita prenatal (p < 0,001). Hubo una mayor prevalencia de BPN en neonatos de sexo femenino (p < 0,001) con madres de edad ≥ 40 años (10,8%; p < 0,001). Los neonatos con buena vitalidad tuvieron una baja prevalencia de BPN (p < 0,001). La frecuencia de las variables estudiadas aumentó al comparar el inicio y el final del período y si las diferencias son estadísticamente significativas. Conclusiones: El estudio llama la atención sobre la necesidad de intervenciones para mejorar los indicadores que determinan el BPN. Arch Latinoam Nutr 2024; 74(2): 74-82.
Palabras clave: Nacimiento vivo, sistemas de información en salud, estadísticas vitales, recién nacido de bajo peso.
https://doi.org/10.37527/2024.74.2.001
Author for correspondence: Jane Laner Cardoso, e-mail: [email protected]
Since the characteristics of the newborn (NB) and the mother, including pregnancy and childbirth, are important to monitor health actions and formulate public policies, the Ministry of health of Brazil established the Information System on Live Births (ISLB) in 1990. The data in the ISLB are based on live birth certificates issued by the health service after childbirth, characterizing the conditions of pregnancy, childbirth, and delivery (1,2).
The Health Surveillance Secretariat of the State Health Secretariats of Brazil manage this at the national level and in the respective states and municipalities, respectively. Declaration of Live Birth (DLB) is the standard document used throughout Brazil to collect data on live births (LBs) (3).
Santa Catarina (SC), located in the southern region of Brazil, has a demographic density of 73.90 inhabitants per km² distributed in 295 municipalities. In Brazil, the fertility rate was 1.75 children per woman, and the infant mortality rate was 9.5 deaths per 1,000 LB, which decreased as shown by the state. These mortality-determining factors involve antenatal and hospital care qualities during childbirth. The collection of information through the Live Births System records helps to monitor progress, identify areas in need of intervention and guide public health policies. (4-6).
Therefore, this research evaluated the DLBs in 2010–2019 obtained from the ISLB database for SC and described the epidemiological profile of LB and obstetrics in 2010–2019, thereby identifying the profile of newborns, maternal characteristics related to the delivery of LB, and the prevalence and profile of newborns with low birth weight (LBW) in pregnancies.
This cross-sectional study described and analyzed the maternal and neonatal characteristics of 940,059 cases of LB in SC in 2010–2019. The period was selected for evaluation because of the series with data corrected by surveillance, considering the beginning of the study in 2021. To determine which factors influenced the behavior of the data series, a consistent database is essential.
The variables related to the mother, pregnancy, and NB were analyzed. Moreover, the variables related to the mother and pregnancy included the mother’s age group in years, education in years, race/color, and marital status. The proportion of LBW during a term was evaluated, and the factors associated with LBW were investigated according to maternal age categories. Other factors included the number of previous pregnancies, living children, fetal losses and miscarriages, and normal and cesarean deliveries; number of pregnancy weeks; antenatal consultations; month, in which antenatal care started; type of pregnancy and delivery; type of presentation of the newborn; induced labor; commencement of cesarean section before labor began; and the attendees at the time of birth (doctor, nurse/midwife, midwife, and other).
The variables related to mother and pregnancy were: mother's age group (10 to 19 years, 20 to 24 years, 25 to 29 years, 30 to 34 years, 35 to 39 years, 40 years or more); mother's education (none, 1 to 3 years, 4 to 7 years, 8 to 11 years, 12 and more); mother's race/color (white, black, yellow, brown, indigenous); mother's marital status (single, married, widow, legally separated, stable union); number of previous pregnancies (none, one, two, three, four, five or more); number of living children (none, one, two, three, four, five or more); number of fetal losses and miscarriages (none, one, two, three, four, five or more); number of normal births (none, one, two, three, four, five or more); number of cesarean deliveries (none, one, two, three, four, five or more); weeks of gestation (less than 22 weeks, from 22 to 27 weeks, from 28 to 31 weeks, from 32 to 36 weeks, from 37 to 41 weeks, from 42 weeks and more); number of prenatal consultations (none, 1 to 3, 4 to 6, 7 and more); month of start of prenatal care (first, second, third, fourth, fifth or more); type of pregnancy (single, double, triple or more); type of birth (vaginal, cesarean section); type of newborn presentation (cephalic, pelvic, transverse); induced labor (no, yes); cesarean section occurred before labor started (no, yes); who attended the birth (doctor; nurse/midwife, midwife, others).
The variables related to the NB were gender, race/ color, 1-min and 5-min APGAR scores (good vitality: scores of 7–10, moderate asphyxia: scores of 4–6, and severe asphyxia: scores of 0–3), identified anomalies, and LBW (weight below 2,500 grams) (6,7).
Data were described using absolute (n) and relative (%) frequencies for categorical variables. The exclusion criteria adopted were variables that behaved as outliers, with quantitative variables identified with possible errors or inconsistencies being considered as such. To ensure information quality, outliers were excluded from the analysis (8).
The frequency of the variables studied was also checked, comparing the beginning and the end of the period (2010-2019).
Quantitative variables were categorized or described using central tendency analysis (mean, median, and standard deviation [SD]).
Either Pearson’s chi-squared test or Fisher’s exact test was used to test the hypothesis of the relationship between maternal and pregnancy variables and NB with birthyear and assess the difference in proportions between LBW and maternal age groups in term infants. Analyses were considered statistically significant if p < 0.05. Data were presented in a Microsoft Excel spreadsheet and analyzed using IBM SPSS 25 software.
This research was submitted to the Research Ethics Committee of the School of Public Health of the State and Health Department of Santa Catarina and received a favorable opinion (number: 5,079,025) in November 2021.
Table 1 describes maternal, pregnancy, and neonatal characteristics using quantitative variables. The mean maternal age was 27.1 years (SD = 6.5, range 10–64 years); the number of LBs and the mean number of fetal deaths and abortions were 0.9 and 0.2, respectively; gestational age was 38.5 weeks (SD = 2.2) and the mean number of antenatal consultations was 8.1; the mean month of initiation of antenatal care was 2.5 months (SD = 1.3); and birth weight was 3,217 grams (SD = 552.3) and the median was 3,250 grams.
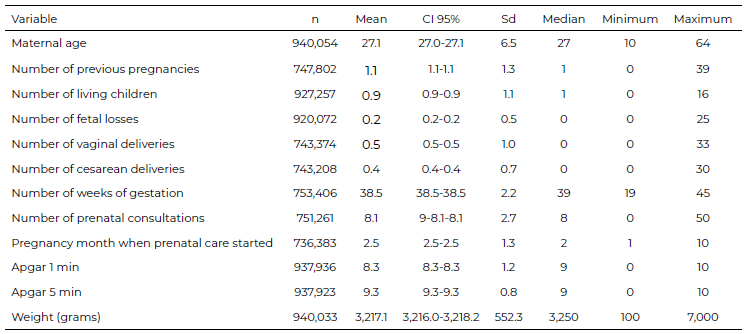
Table 2 shows the prevalence of LBW in full-term pregnancies (37–41 weeks of gestation) according to maternal age group and other variables. It was higher among mothers without education (none) and black women than mothers with 12 or more years of education (p < 0.001). The prevalence of LBW was also high in pregnancies of mothers without antenatal care (p < 0.001), those aged 40 years or over (11.8%), and mothers who had antenatal care from the 5th month of pregnancy onward.
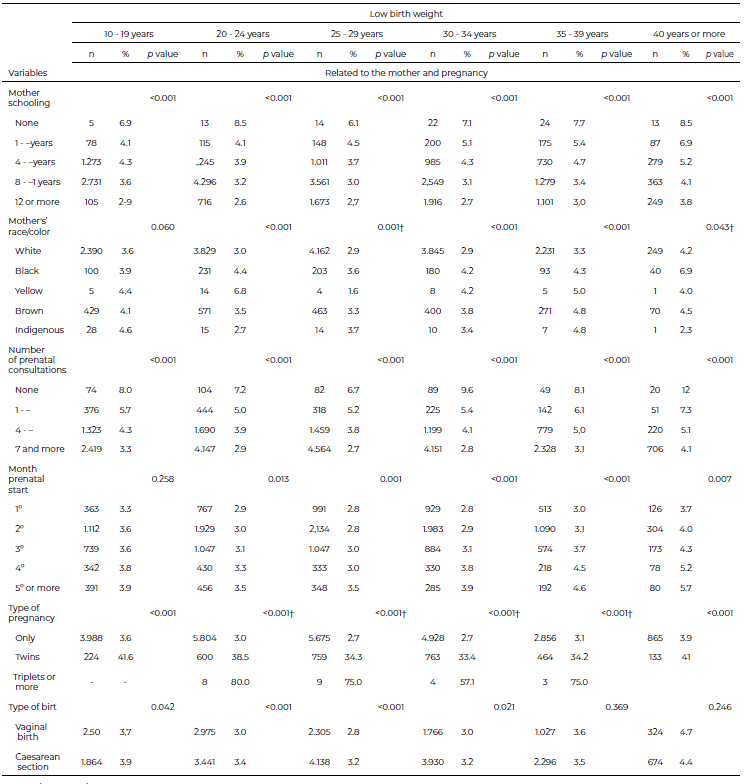
The frequency of low birth weight was 7.8% on average, with slight variations (7.8 to 7.9%) throughout the decade studied.
Table 3 shows the prevalence of LBW according to the maternal age group and characteristics of the newborn. This was high in female newborns (p < 0.001) and in those with an identified anomaly (p < 0.001), and these differences were observed for all maternal age groups. In addition, neonates with good vitality on the APGAR scores at 1 and 5 minutes had a low prevalence of LBW (p < 0.001).
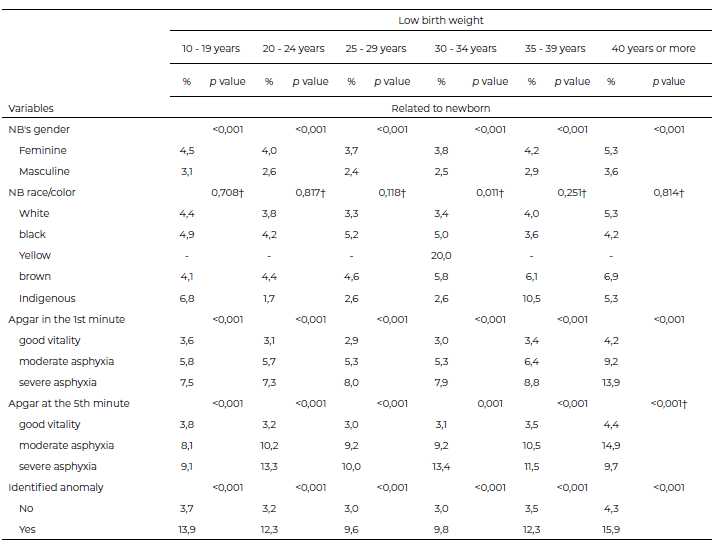
The frequency of LBW was high in NB of women aged 40 years or older (4.5%) and low in those aged 25–29 years (3.0%) (p < 0.001).
During the decade studied, there was a higher frequency of mothers aged 35 to 39 and 40 or over, an increase in the percentage of mothers with 12 or more years of schooling of brown race/color, and with a stable union. There was also an increase in the frequency of women with one living child, with a fetal loss and miscarriage and with a cesarean delivery and an increase in the percentage of women with 7 or more prenatal consultations, as well as a higher frequency of women who started prenatal care in the first month of pregnancy. Double pregnancies increased, as did the frequency of vaginal deliveries, although cesarean deliveries were more frequent in all years. Regarding newborns, there was an increase in the frequency of white births, but the frequency of low birth weight remained practically unchanged during the period (7.8 to 7.9%). Most newborns showed good vitality on the 1st minute and 5th minute Apgar scores.
The differences in frequencies between the beginning and end of these variables were statistically significant (p<0.001), except for birth weight (p=0.103).
In relation to gestational age, the profile of LB showed that most were born at term (87.09%), preterm (10.90%), and post-term (1.60%); most mothers had seven or above consultations (69%); however, 67.43% underwent cesarean section. Correlating LBW with gestational age and schooling, 70.28% of LB with insufficient or LBW were of appropriate gestational age, and 39.44% had been educated between 8 and 11 years.
To make proper public health decisions we must rely on reliable and timely data on births and deaths, including cause of death, which is best collected through a well-functioning civil registration and vital statistics system. Statistics on births and low birth weight are important indicators for assessing public health and child well- being in the Americas. The most recent data on births in the Americas varies significantly between countries, reflecting differences in population size, fertility rates and health policies (9).
In the United States of America (USA), a study evaluating data from the 2013–2014 Annual Vital Statistics (10) found that the number of births increased by 1% between 2013 and 2014; the total fertility rate increased by 1% (62.9 births per 1,000 women); and the teenage birth rate reached an all-time low in 2014 (24.2 births per 1,000 women).
In this study, the prevalence of LBW was higher among mothers without education (none) than mothers with 12 or more years of education (p < 0.001). There was also a high prevalence of LBW among mothers who had no antenatal care (p < 0.001) (11.8% among mothers aged 40 years or more) and those who had antenatal care after 5 months of pregnancy. There was a high prevalence of LBW in female neonates (p < 0.001) and neonates with an identified anomaly (p < 0.001), and these differences were observed for all maternal age groups. Moreover, neonates with good vitality on the APGAR scores at 1 and 5 minutes had a low prevalence of LBW (p < 0.001) (Table 2).
This study considers preterm labor in a regular uterine contraction between 20 and 36 6/7 weeks’ gestation, with subsequent Preterm birth mainly causing perinatal morbidity and mortality (11). Cesarean section is generally not recommended before 39 weeks of gestation due to the increased risk of respiratory morbidity in the baby (strong recommendation) (12).
Regarding the risks of choosing an elective cesarean section, a cohort study of all women in Canada (13) found that the risks of major maternal morbidity associated with planned cesarean section are greater than those associated with planned vaginal delivery.
A study reviewing cesarean section rates in 150 countries (14) shows that 18.6% of all births are currently cesarean, with rates ranging from 6% to 27.2% in developing and developed regions, respectively. The authors conclude that the recommendation for cesarean section has increased to unprecedented levels worldwide, although the difference between populations of high and low socioeconomic levels remains, highlighting the need to propose global and regional policies and strategies to reduce cesarean section rates.
Brazil has also seen a significant increase in cesarean section rates in recent decades, even higher than in the study cited above (55.7% of births). Possible reasons for this are improved access for women to surgical procedures for cesarean section and medical indication without technical criteria (15).
Another important point is the increased frequency of advanced maternal age. Defined as when the age at birth is ≥35 years; very advanced when the age is ≥45 years. With advancing age, the risk of maternal and fetal complications increases, and so does the potential risk of intrapartum morbidity and mortality from venous thromboembolism, obstetric hemorrhage, shock, stroke, and heart failure (16-18).
In Brazil, studies aimed to evaluate the frequency of late pregnancy (19,20) found that the fertility rate by age, the rate of prematurity, and LBW were associated with advanced maternal age. It concluded that the birth frequency and specific fertility rate for age ≥35 years increased between 1995 and 2018, increasing the likelihood of prematurity and LBW.
Also, an investigation of the association between antenatal care adequacy and LBW outcomes, evaluating 368,093 LB at term at the ISLB in Brazil, concluded that LBW was likely associated with young mothers. Also, LBW was associated with advanced maternal age, unmarried women, black or brown ethnicity, low education, primiparous, previous preterm birth, and female newborns (21.22).
Although many women delay pregnancy to pursue educational and career goals, some studies (12,15,23) suggest a risk for infertility, pregnancy loss, fetal abnormalities, dystocia, stillbirth, and obstetric complications due to advanced age. A population- based cohort study using the UK Obstetric Surveillance System (24) from UK hospitals found that the high risk of complications in pregnancy with advanced age is attributed to multiple pregnancies or the use of assisted conception.
Regarding prematurity, a study in Brazil (2012 and 2019) (25) evaluated variables like those in this study (maternal age, maternal education, race/color, number of prenatal consultations, and mode of delivery) in data from the ISLB. Women aged ≥45 years and with 4–6 antenatal consultations had the highest proportion of preterm births at an increasing trend. There was a decreasing trend for illiterate and indigenous women, although they had the highest proportions of preterm birth over the period. The study concluded that there is a decreasing trend in preterm birth, especially among women from vulnerable groups.
However, a national survey (16) in the ISLB database showed that cesarean delivery rates were higher than those recommended by the Ministry of Health, with cesarean delivery being associated with maternal age >35 years and a high number of prenatal consultations.
In this study, the mean gestational age was 38.5 weeks (SD = 2.2), and the mean number of antenatal consultations was 8.1 over the period analyzed, which may indicate the quality of antenatal care. Regarding birth weight, the mean was 3,217 grams (SD = 552.3) and the median was 3,250 grams (Table 3).
In our study, a higher percentage of LBW was observed among NB of women aged 40 years or older (10.8%) than that of women aged 10–19 years (8.5%), and this difference was statistically significant (p < 0.001).
The temporality of the frequency of the variables studied was also checked, comparing the beginning (2010) and the end of the period (2019), and there was an increase in all frequencies and these differences were statistically significant, except for birth weight, which hardly changed at all. A study describing the temporal trend of maternal, healthcare and newborn characteristics in the state of Rio de Janeiro. showed similar results: there was an increase in mothers over 35, an improvement in schooling, with a reduction in the percentage of pregnant women with less than eight years of schooling, and an increase in women who had seven or more prenatal consultations. Cesarean deliveries showed an upward trend and low birth weight showed a downward trend of 1.1% per year (26).
This study has some notable limitations that can be used to improve ISLB data records. This database has a total of 940,059 LBs from 2010 to 2019 in SC. This research showed variables behaving like outliers and those that were transformed into missing ones, which include the number of living children, dead children or abortions, previous pregnancies, normal deliveries, cesarean deliveries, prenatal consultations, and maternal schooling (0.005% of the total data). The variable "normal births" had the highest number of outliers. Another important limitation is that all the analyses carried out were based on the variables contained in the ISLB databases, since the aim of the study was to analyze these data. Thus, for example, other maternal comorbidity factors, such as obesity, hypertension, and diabetes, which can interfere with low birth weight, were not included in this study.
Also, which analyzes vital statistics, shows descriptively the behavior of variables in the live birth system, and could contribute to public health in the state of Santa Catarina, Brazil. Despite the favorable evolution of data records in ISLB databases, the importance of developing studies to find new evaluation forms to improve the system’s quality is highlighted. However, these results are of utmost importance for health services, as they indicate that women in extreme reproductive age are more susceptible to adverse perinatal outcomes, and are therefore, emphasizing the need for adequate care planning that should be given to them to these women.
Finally, this study concludes that the maternal and neonatal indicators, in relation to the analysis of the averages, concur with normal parameters. Advanced maternal age, low education, lack of access to prenatal care and its late start, female sex, and the presence of anomalies are associated with LBW. This analysis may improve maternal and child health.
The authors declare that they have no conflicts of interest
Recibido: 13/03/2024
Aceptado: 21/05/2024